The value-based modifier (VM) program was created under the Affordable Care Act and requires that the Centers of Medicare & Medicaid Services (CMS) apply VMs in determining physician pay for services performed under Medicare Part B-a process that has already begun its rollout in early 2015 (see below for important dates and deadlines).1 Yet with the VM rollout scheduled to be completed in 2018, many are left to wonder what affect VMs will have on eligible professional (that includes physicians, CRNAs, PAs, NPs, and CNSs) pay? Herein we aim to dive into some of the common questions surrounding VMs and predict what affect VMs will have on healthcare providers.
The most important aspect of the VM program is to note is that it is a departure from the traditional fee-for-service model (a volume centric model) employed by CMS in determining physician pay2. In other words, provider pay will not be determined solely by the number of patients seen in a given time period. Instead the VM program aims to incentivize providers to improve the quality of their care in order to receive higher levels of compensation. Simply put, the value modifier acts to increase/decrease a provider’s compensation based on the quality of service, rather then the number of patients seen. This implies, for example, that an anesthesia services provider, or anesthesia management provider that traditionally sees 400 patients/day would focus on improving the quality of care for those patients rather than trying to scramble and see extra patients(the rationale stemming from the idea that physicians and other healthcare professionals can deliver higher quality care if they are not pressured to see more patients).
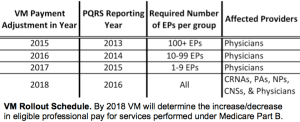
This shift from a volume-centric model toward a quality-based model raises a couple of natural questions: how are physicians and other eligible providers evaluated for the quality of care? What quality metrics would be employed? Are payments based solely on the quality of care? These questions address many of the common misconceptions about VMs. For example, VMs take into account the cost and quality of rendering a service in determining payment-not just the quality of care. To measure quality, CMS relies on a system known as the PQRS (Physician Quality Reporting System). The PQRS program is a quality reporting program that encourages individual eligible professionals (EPs) and group practices to report information on the quality of care to Medicare.3 This means that physicians and other eligible professionals may elect to report on certain aspects of care delivered (i.e. the use of Post Anesthesia Care Unit-PACU- guidelines). Based on the relationship of the quality of care delivered with respect to other providers the provider may be eligible for an upgrade/downgrade in pay. One final factor to note is that the quality metrics reported in a given calendar year affect VM adjustment in the following two years, as noted in the table. Thus PQRS reports in 2016 will affect VM adjustment in 2018.
In the context of our earlier example, of an anesthesia services provider, or anesthesia management provider, this group could choose to report on self-selected measures of quality. For example, the group could report on the use of PACU guidelines, the percentage of smokers who abstain from smoking prior to anesthesia, and perioperative temperature management in assessing the quality of care delivered. These quality metrics are then compared to similar anesthesia services providers and the providers are ranked on the basis of quality of care delivered and the cost of care delivered. This combined cost-quality of care metric is then used to determine the VM. Groups with high cost of care and low quality of care are penalized by up to -4% (a 4% downgrade in pay), while groups that deliver high quality care at lower cost are rewarded with a +4% boost in pay. The use of penalties in VMs brings an important note about the VMs to the surface. The CMS designed the VM system is designed to be globally budget-neutral so that the national incentive pool equals the size of the penalty pool. Hence, high-performing professionals are in essence rewarded with dollars taken from low-performing professionals.2
This financial penalty/reward system brings about many concerns about the future quality of care and the overall makeup of healthcare providers. We predict the increased use of CRNAs and PAs to decrease the cost of service while maintaining a similar level of care (the idea being that physicians may command higher levels of pay for similar services). In addition, we predict two broad changes in healthcare delivery. The first is consolidation of healthcare provider groups in order to achieve higher quality of care while reducing fixed costs of healthcare delivery; the second is the increased deviation of high performing physicians/physician groups from performing services under Medicare Part B. Nonetheless, as the VM program takes full effect in early 2018, the quality of healthcare will be closely monitored and the advantages/disadvantages of the VM system will be evaluated.
References:
- http://www.aana.com/resources2/quality-reimbursement/Pages/Value-Based-Modifier.aspx
- http://www.saignite.com/resources/10-faqs-about-pqrs-and-the-value-based-payment-modifier
- https://www.cms.gov/medicare/medicare-fee-for-service-payment/physicianfeedbackprogram/valuebasedpaymentmodifier.html

