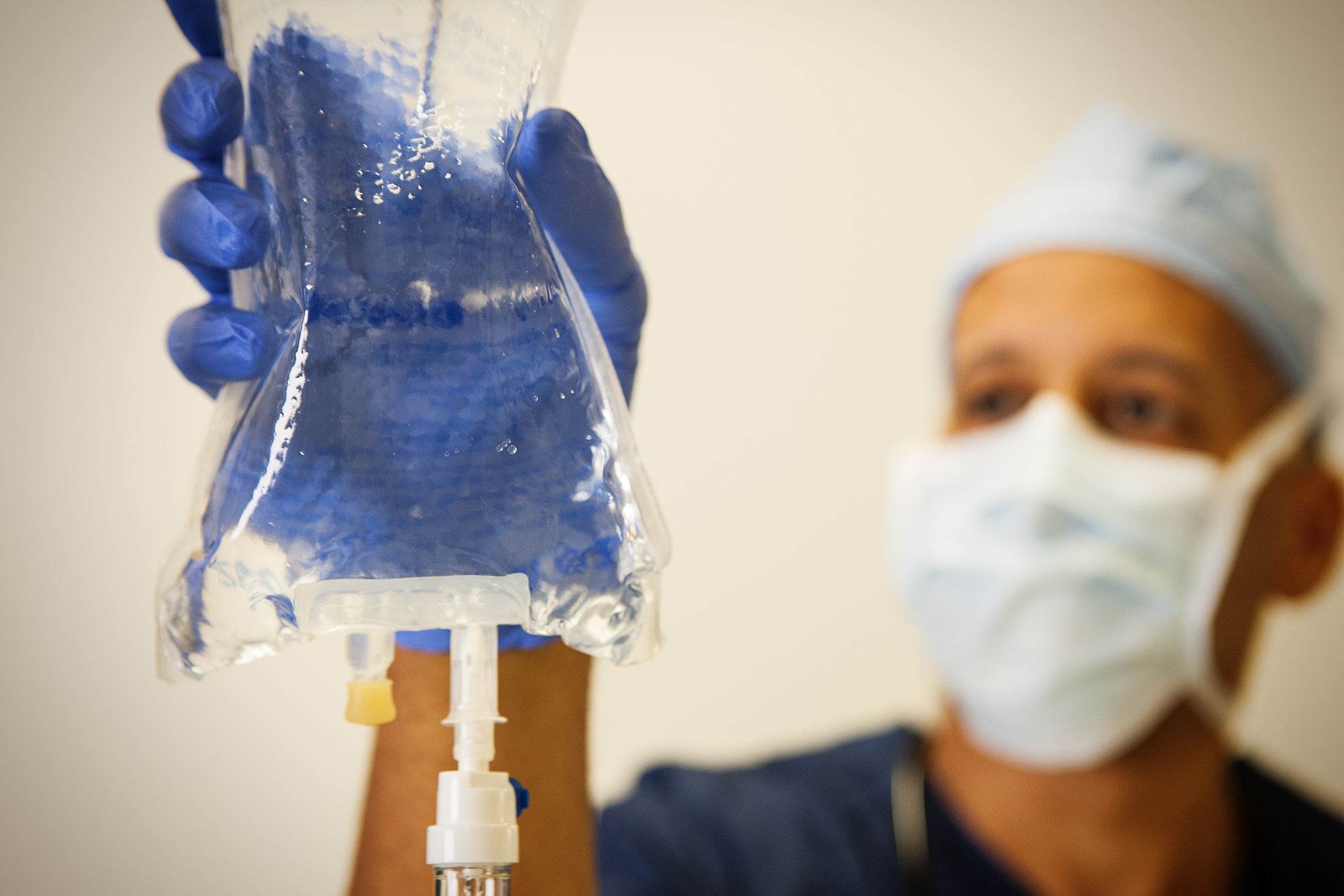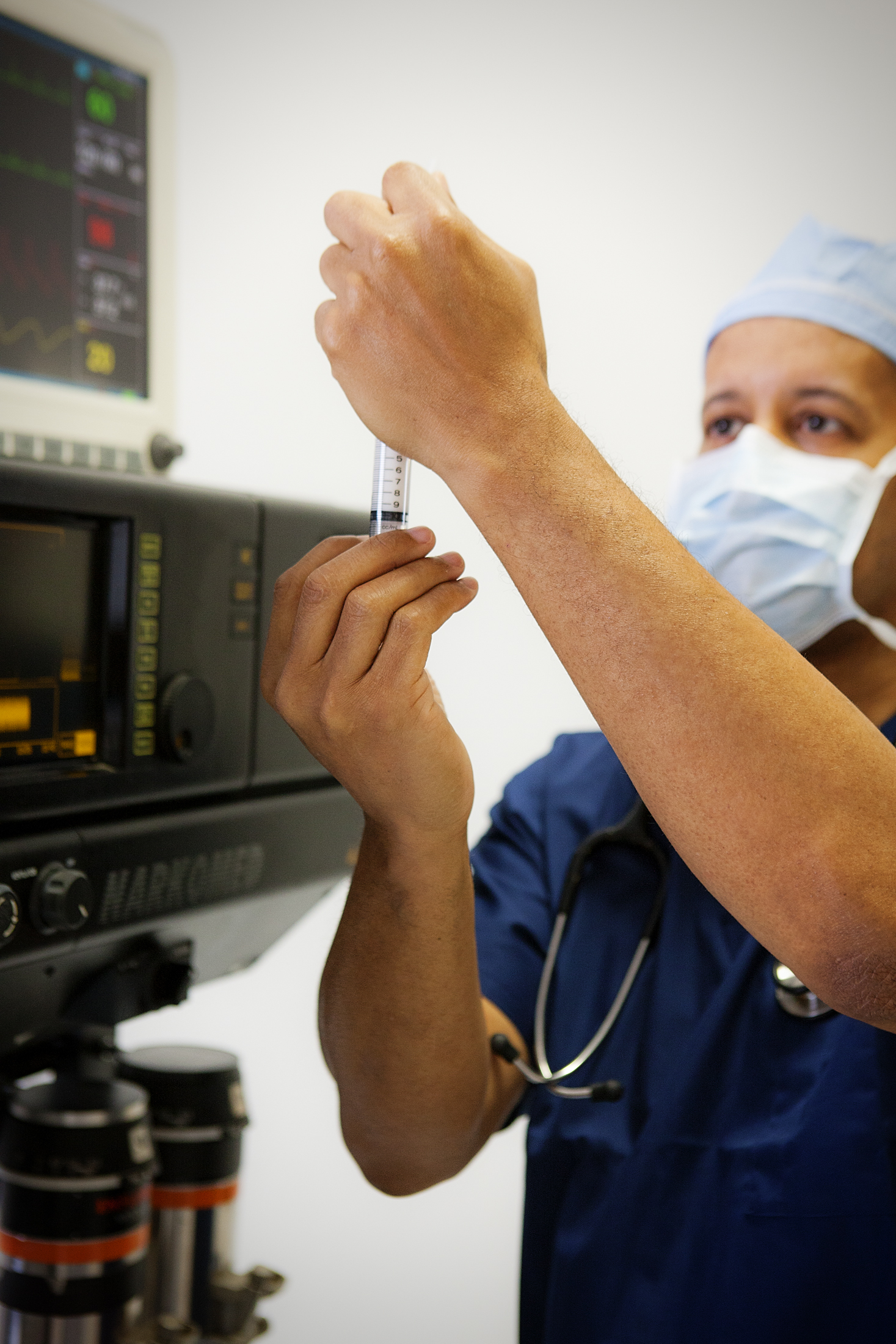
Recent advances in telehealth promise to improve health outcomes – and save both time and money. Using a wide variety of technological innovations, practitioners using telehealth can provide consultations, conduct check-ups, and perform procedures, all without meeting a patient face-to-face.
In former decades, “telehealth” mostly meant using a phone to call your doctor. Now, doctors can perform even complex robotic surgeries on patients who are on the opposite side of the world. With digital medical equipment, cameras, and video chatting, doctors can evaluate and treat patients without meeting them in person. These methods are not only cost-effective, but also improve upon current health procedures: recent studies of telehealth implementation show that incorporating technology into health care services can actually lead to better medical care even while cutting costs.
In rural or sparsely populated areas, where specialists are few and far between, telehealth can provide enormous benefits to long-underserved populations. In a study begun in 2014 in Sunflower County, a poor area of Mississippi, using telehealth for 100 patients led to the discovery of 18 cases of diabetic retinopathy that would otherwise have gone undiagnosed, and saved patients a collective 10,000 miles of travel.
In anesthesia services, remote consultations and procedures are already saving people time and money. Instead of meeting patients face-to-face before a procedure, anesthesiologists can conduct a full physical exam by video. In one recent study, a nurse present with the patient used an airway camera to enable doctors to conduct a full airway exam of the respiratory system, and used a digital stethoscope to enable full heart and lung auscultation. Using this equipment eliminates the need for a pre-operative meeting, so that patients and doctors meet only on the day of the procedure. By reducing the amount of in-person interaction between doctor and patient, telehealth pre-operative anesthesia services appointments have the potential to cut Medicare spending in this sector.
Doctors can even administer and manage anesthesia from afar. In one study, anesthesiologists remotely controlled intravenous anesthesia using an automated system called the “Anesthesia Cockpit.” This system controls the anesthesia’s impact on the patient by adjusting the drug level according to physiological indicators like heart rate, blood pressure, and level of consciousness.
More and more practitioners are incorporating these new technologies into their standard operations. In 2015, there was a 25% increase in total Medicare payments for telehealth from the previous year. According to a 2015 National Business Group on Health survey, in 2016, 74% of large employers expect to offer telehealth services to their employees. The latest report by business intelligence provider GBI Research claims that telehealth has the potential to yield over $6 billion in healthcare savings every year. Given the fact that, according to the Center on Budget and Policy Priorities, Medicare spending along with Medicaid, CHIP, and Affordable Care Act marketplace subsidies accounts for 25% of the federal budget (some $900 billion), the potential of telehealth to cut government health insurance spending has real significance.
But certain barriers still prevent telehealth from reaching its full potential. Communicating through video chat or other web-based means often requires sending personal medical data across a connection, and thus data security and privacy are issues. In developing countries and other areas where IT literacy is low, it is difficult to implement telehealth practices without encountering technological difficulties.
In addition to these issues inherent to telehealth, there are larger features of the medical system that have slowed its progress. Restrictions on Medicare reimbursements limit in what circumstances doctors may receive payment for conducting appointments and procedures over the Internet. Many states – including Texas, Arkansas, Mississippi, Alaska, Alabama – have recently upheld legislation that mandates face-to-face meetings in certain situations, thereby reducing the potency of telehealth solutions. Although there has been progress at the state level – just this week, the Texas State Board of Examiners of Professional Counselors rejected a proposal to mandate that therapists establish an in-person relationship with a patient before turning to telehealth – significant systemic barriers still exist.
But the federal government may lower some of these barriers soon. Just over a month ago, a bipartisan group of senators introduced a bill, the “CONNECT for Health Act,” which proposes to expand the scope of Medicare reimbursements for telehealth and remote patient monitoring services. An identical bill was introduced in the House of Representatives just a couple of days later. An independent report predicts that the bill would save the federal government $1.8 billion over the next ten years, if it passes through Congress.
Although telehealth is far from reaching its full potential, it is certainly on the rise. It’s worth keeping an eye on the news from this sector of the health care system to see what’s next in the world of digital health, and how these new techniques can both lower costs and promote good health