



Traditionally, NPO guidelines were established to reduce the risk of aspiration and other complications during anesthesia by restricting food and liquid intake prior to surgery. NPO guidelines have evolved over time, particularly with the growing understanding of the safety and implications of allowing certain oral medication closer to surgery time. Current evidence suggests that permitting oral medications with a small sip of water up to two hours before surgery does not significantly increase aspiration risk and may improve patient outcomes (1).
NPO guidelines have traditionally required patients to abstain from all food and liquids, including oral medication, beginning at midnight prior to surgery. However, this approach has been increasingly questioned due to the potential negative effects on patient well-being, such as dehydration, hypoglycemia, and increased anxiety, along with potential impacts from medication stoppage, which may subsequently affect surgical outcomes (1). Updated NPO guidelines now advocate a more nuanced approach, particularly with regard to oral medications that are critical to the management of chronic conditions. Medications for conditions such as hypertension, asthma, and heart disease can lead to perioperative complications if withheld; therefore, their continuation with minimal water intake is often recommended (2).
Current research supports the administration of certain oral medications preoperatively, as long as they are taken with a small amount of water – typically 30 ml or less – within two hours of surgery. This approach is not considered a violation of NPO guidelines and aims to strike a balance between minimizing the risk of aspiration and avoiding exacerbation of underlying medical conditions (2). For example, patients taking beta-blockers for cardiac conditions should generally continue their medication to avoid adverse cardiovascular events associated with sudden withdrawal.
Despite the evidence, application of updated NPO guidelines varies widely among institutions and practitioners. Resistance to change is due, in part, to ingrained practices and the slow adoption of new guidelines into routine clinical practice. Surveys of U.S. hospitals have revealed significant discrepancies between current evidence and clinical practice, with many providers still adhering to “NPO after midnight” rules (3). Such outdated practices can negatively impact patient safety and comfort, highlighting the need for ongoing education and dissemination of guidelines to ensure that evidence-based practices are followed.
In addition, the debate around NPO guidelines extends beyond medications to include other forms of oral intake, such as clear liquids, which some recent studies have shown can be safely consumed up to two hours before surgery without increasing the risk of aspiration (Wilson, 2017). This evolving understanding emphasizes the importance of individualized patient care, where decisions about preoperative medications and fluid intake are tailored to the patient’s specific medical conditions, type of surgery, and anesthetic requirements.
The administration of preoperative oral medications under NPO guidelines should be approached with an evidence-based mindset that allows for necessary medications with minimal fluid intake close to surgery. This approach minimizes the risks associated with omitting critical medications, while maintaining the fundamental goal of preventing aspiration. Consistent updating and dissemination of NPO guidelines to healthcare providers is essential to bridge the gap between research and clinical practice, ultimately improving patient safety and surgical outcomes.
References

Driven by changing market dynamics and a growing provider shortage, the field of anesthesia has sustained significant upheaval in recent years. These shifts, characterized in part by large, consolidated anesthesia firms replacing local groups in hospital systems, represent an unprecedented departure from traditional anesthesia field practices, with significant implications for anesthesia providers and their patients.
One of the major underlying causes of these shifts in the landscape of anesthesia groups — the national anesthesia provider shortage — is not new. In the early 2000s, the demand for anesthesia providers began to outgrow the supply (1). The aging American population that required more procedures and the expansion of hospital surgical staff across the country put pressure on the medical field, which responded by increasing residency positions by 12% and increasing medical school class sizes (1, 2). Despite these efforts, demand has continued to outpace supply, with over half of anesthesiologists over the age of 55, signaling an impending exodus of retirees that will exceed the influx of younger anesthesiologists (1). While the number of physicians in other specialties have grown an estimated average of 7% between 2016 and 2021, anesthesiologists have increased by only 1%, leading to an expected shortage of 12,500 in 2033 (3). This shortage has resulted in increased wait times for routine and urgent procedures, financial impact on hospital systems and anesthesia firms, and provider dissatisfaction (4).
In the wake of this shortage and its negative impacts on hospital systems, a new form of anesthesia firm management has emerged, represented by the wave of consolidation (5). This new form — large, consolidated anesthesia groups purchased, assembled, and directed by national for-profit healthcare organizations or private equity firms — has rapidly grown from roughly 3% of all anesthesia firms in 2009 to nearly 19% in 2019 (6). This percentage has increased due to large companies’ and private equity firms’ interest in highly specialized, relatively expensive medical specialties — including anesthesia groups, dental offices, and ophthalmology clinics — due to their high profit margins (7). Historically, hospital systems have staffed anesthesia services by contracting with local firms, but these new, large, consolidated firms appear attractive to hospitals, with promises of adequate staffing and decreased cost (7). In fact, between 2023 and 2024, more than 10 large hospital systems across the country severed ties with local firms and entered contracts with consolidated groups, representing an unprecedented shift in the anesthesia industry (8).
Unfortunately, some of these groups have been unprepared, resulting in worsened shortages, exorbitant surgery wait times, and criticism (9, 10). For example, in 2023, a hospital system in Oregon suddenly terminated its agreement with a local group and began contracting with a consolidated group backed by a private equity firm (10). Despite appearing more efficient, the new firm had cut necessary costs and jobs, resulting in a massive anesthesiologist shortage and a significant delay in surgeries (10).
Despite hospitals’ increasing preferences for ostensibly lower-cost, better-staffed consolidated anesthesia groups, shifts toward this model has been met with scrutiny from anesthesia providers, their communities, and the federal government. For example, in Texas, two private equity firms allegedly colluded to consolidate anesthesia firms across the state to create a monopoly, eliminate local groups, and hike up prices for hospitals and patients, resulting in the Federal Trade Commission filing lawsuits against the firms in 2023 (11). This lawsuit represents many anesthesia providers’ sentiments about the wave of consolidation, with many critics arguing that this shift from local physician-managed firms to national corporation-managed groups results in higher costs for patients, lower-quality care, job losses, and the pursuit of profits at the expense of patients and their providers (7, 12). The future of the industry remains unclear as many hospital systems evaluate the performance of their contracted anesthesia groups.
References
1: Menezes, J. and Zahalka, C. 2024. Anesthesiologist shortage in the United States: a call for action. Journal of Medicine, Surgery, and Public Health, vol. 2. DOI: 10.1016/j.glmedi.2024.100048;
2: American Association of Medical Colleges (AAMC). 2024. “Physician specialty data report.” AAMC Data and Reports. URL: 2016-2021https://www.aamc.org/data-reports/workforce/data/percentage-change-first-year-acgme-residents-fellows-specialty-2016-2021.
3: Kaplan, K. and Polanco, K. 2023. “Where have all the anesthesia specialists gone? Insights for healthcare leaders.” Veralon Healthcare Management Advisors. URL: https://www.veralon.com/wp-content/uploads/2023/10/Veralon-Blog-Where-Have-All-the-Anesthesia-Specialists-Gone-Insights-for-Healthcare-Leaders-Oct2023.pdf.
4: Peters, J. 2022. The physician leader’s role in navigating the anesthesia provider shortage. American Association for Physician Leadership, vol. 9. DOI: 10.55834/plj.9178639149.
5: Paone, J. 2022. “Trend to watch: inside the consolidation of anesthesia services.” Outpatient Surgery Magazine. URL: https://www.aorn.org/outpatient-surgery/article/2022-February-anesthesia-services.
6: Adler, L., Milhaupt, C. and Valdez, S. 2023. Measuring private equity penetration and consolidation in emergency medicine and anesthesiology. Health Affairs Scholar, vol. 1. DOI: 10.1093/haschl/qxad008.
7: Kotsonis, S. and Chakrabarti, M. 2023. “How private equity is changing American health care.” WBUR. URL: https://www.wbur.org/onpoint/2023/11/07/how-private-equity-is-changing-american-health-care.
8: Hollowell, A. 2024. “Why US hospitals are breaking up with anesthesiology groups.” Becker’s Hospital Review. URL: https://www.beckershospitalreview.com/care-coordination/why-us-hospitals-are-breaking-up-with-anesthesiology-groups.html.
9: Coleman, A. 2024. “Methodist delays surgeries after breakup with anesthesia provider.” WREG. URL: https://wreg.com/news/local/methodist-delays-surgeries-after-breakup-with-anesthesia-provider/.
10: Newitt, P. 2024. “Oregon hospitals’ surgeries plummet amid anesthesiologist shortages.” Becker’s ASC Review. URL: https://www.beckersasc.com/anesthesia/oregon-hospitals-surgeries-plummet-amid-anesthesiologist-shortages.html#:~:text=Surgeries%20at%20two%20Providence%20hospitals,equity%2Dbacked%20physician%20staffing%20firm.
11: Federal Trade Commission. 2023. “FTC challenges private equity firm’s scheme to suppress competition in anesthesiology practices across Texas.” FTC press release. URL: https://www.ftc.gov/news-events/news/press-releases/2023/09/ftc-challenges-private-equity-firms-scheme-suppress-competition-anesthesiology-practices-across.
12: Answine, J. 2023. “War games: private anesthesia group versus hospital system versus private equity firm.” OR Management News. URL: https://www.ormanagement.net/Opinion/Article/09-23/War-Games-Private-Anesthesia-Group-Versus-Hospital-System-Versus-Private-Equity-Firm/72302.
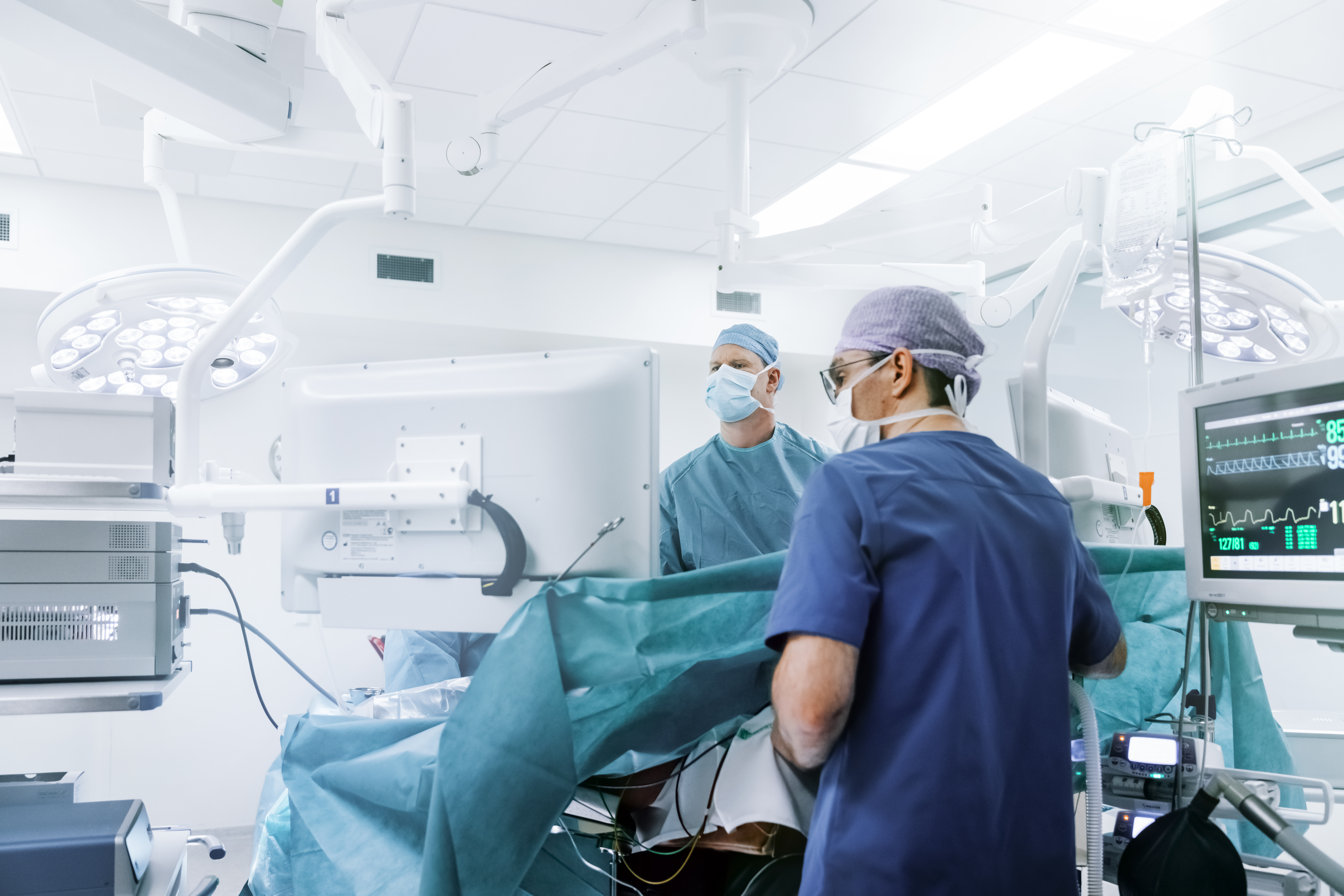
Laparoscopic adrenalectomy for pheochromocytoma is a preferred surgical method due to its minimally invasive nature and associated rapid recovery. However, this procedure poses unique challenges, primarily due to the risk of intraoperative hemodynamic instability. Understanding the causes and effective management of these fluctuations during surgery is crucial for improving patient outcomes and ensuring the safety of the procedure.
Understanding Pheochromocytoma
Pheochromocytoma is a rare tumor of the adrenal glands that secretes excess catecholamines—hormones that significantly influence heart rate and blood pressure. The primary challenge in managing a patient with pheochromocytoma arises from these extreme and unpredictable changes in catecholamine levels, which can lead to severe hemodynamic instability during surgical manipulation of the tumor.
Hemodynamic Instability during Surgery
The main concern during a laparoscopic adrenalectomy for pheochromocytoma is the risk of sudden intraoperative blood pressure spikes and drops. These hemodynamic changes are predominantly triggered by the surgical manipulation of the tumor, causing a massive release of catecholamines into the bloodstream. Additionally, the insufflation of the abdomen with carbon dioxide to facilitate a better surgical view can exacerbate cardiovascular effects by increasing intra-abdominal pressure, which affects venous return and cardiac output.
Preoperative Preparation
Effective management of intraoperative hemodynamic instability begins well before the surgery. Preoperative preparation includes thorough cardiovascular evaluation and stabilization. Patients are often prescribed alpha-adrenergic blockers for at least 10 to 14 days before the surgery to control hypertension and normalize blood volume. Beta-blockers may also be added, but only after adequate alpha-blockade is achieved to prevent unopposed alpha-adrenergic receptor stimulation, which can lead to a hypertensive crisis.
Intraoperative Monitoring
Advanced hemodynamic monitoring is crucial during the surgery. Standard monitoring includes continuous electrocardiography (ECG), direct arterial blood pressure monitoring, and central venous pressure assessment. These measures allow for the immediate detection of hemodynamic changes and facilitate swift interventions. In some cases, additional monitoring techniques such as transesophageal echocardiography can be employed to provide real-time information on cardiac function and volume status.
Anesthetic Management
The choice of anesthesia is critical in managing patients with pheochromocytoma. Anesthetic agents that minimize catecholamine release or have minimal effects on cardiovascular stability are preferred. Volatile anesthetic agents, which can stabilize the myocardium against catecholamine-induced dysrhythmias, are often used. Effective pain management intraoperatively and postoperatively is also crucial to prevent pain-related catecholamine surges.
Pharmacological Interventions
Rapid-acting vasodilators and vasopressors are essential components of the pharmacological arsenal needed to manage blood pressure fluctuations during the operation. Sodium nitroprusside is commonly used due to its quick onset and easy titration properties, which helps manage hypertensive episodes. For hypotensive phases, agents like phenylephrine or norepinephrine are employed to maintain adequate perfusion pressure.
Surgical Technique
The surgical technique also plays a significant role in managing hemodynamic instability. Minimizing tumor manipulation and using precise and controlled movements can reduce the risk of excessive catecholamine release. The laparoscopic approach itself, with smaller incisions and reduced tissue disruption, helps reduce the overall surgical stress on the patient compared to open procedures.
Postoperative Care
Postoperatively, patients need close monitoring as the abrupt cessation of catecholamine secretion post-tumor removal can lead to severe hypotension. Intensive care settings are ideal for postoperative management, where continuous monitoring and timely pharmacological support can be provided until the patient’s condition stabilizes.
Conclusion
Managing intraoperative hemodynamic instability during laparoscopic adrenalectomy for pheochromocytoma involves a multifaceted approach encompassing preoperative preparation, sophisticated intraoperative monitoring, careful anesthetic management, meticulous surgical techniques, and vigilant postoperative care. By understanding the complexities of pheochromocytoma and employing comprehensive management strategies, healthcare providers can significantly enhance patient safety and surgical outcomes. This proactive approach ensures that the benefits of minimally invasive surgery can be safely extended to patients undergoing this high-risk procedure.
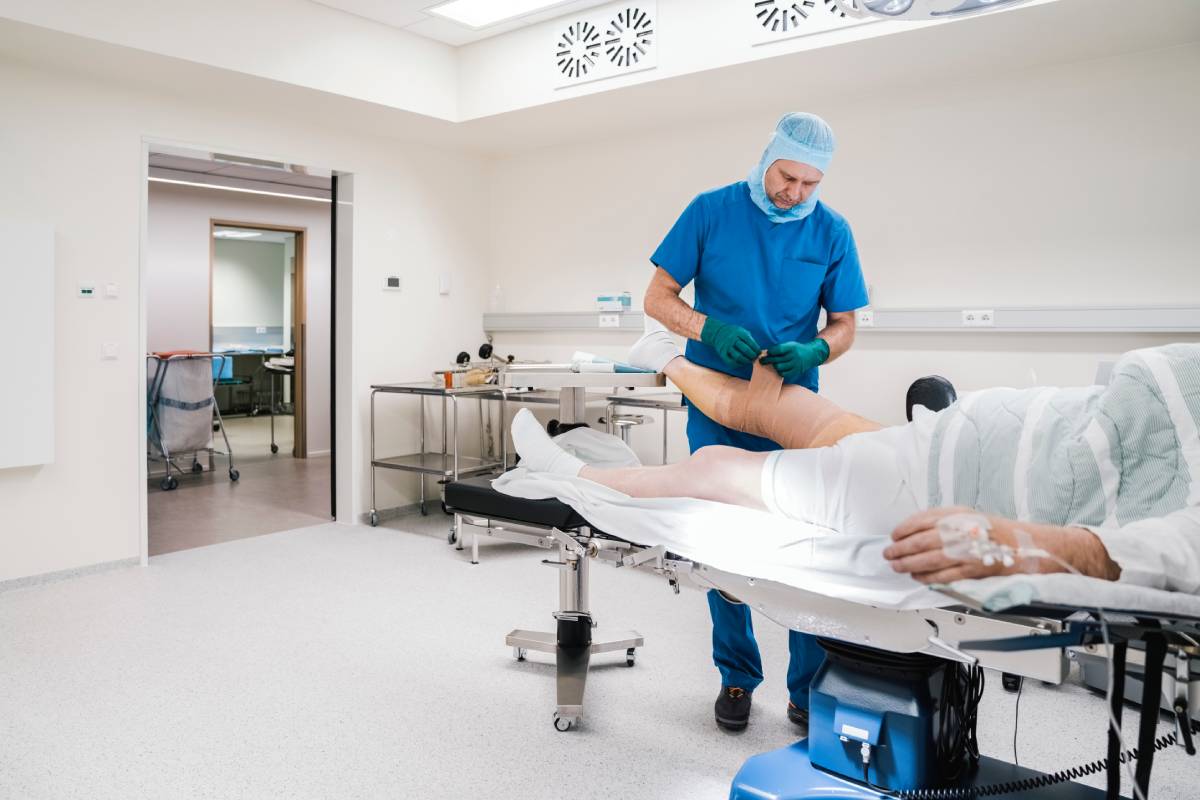
Compartment syndrome is an emergency that can occur during surgery when pressure builds up in an enclosed space of tissue, eventually cutting off blood flow to that area and leading to tissue necrosis. This increased intracompartmental pressure must be reduced quickly through surgical intervention, also known as fasciotomy.
Compartment syndrome most commonly occurs in the anterior compartment of the leg and the limbs in general, but it can also occur in other parts of the body, such as the abdomen. It most often arises after trauma and resulting bone fractures but may also be caused by soft tissue injury, burns, crush injury, overdoses, infection, bleeding disorders, and more. Compartment syndrome can also occur during surgery due to a variety of etiologies (Torlincasi et al., 2023).
Some procedure-related factors that can increase risk of compartment syndrome include duration of surgery, type of surgery, type of anesthesia, and patient positioning. For example, prolonged surgeries can lead to increased external pressure and immobility for patients (Halvachizadeh et al., 2019). Some anesthetic agents can cause hypotension and decreased perfusion pressures. Long-acting regional anesthesia may mask the signs and symptoms of compartment syndrome (Garner et al., 2014). Surgical techniques that require use of tourniquets or increased fluid administration may also increase compartment syndrome risk (Halvachizdeh et al., 2019). Excessive fluid administration can lead to tissue edema and increased intracompartmental pressures.
There are patient risk factors that can also increase the likelihood of compartment syndrome during surgery. For example, patients with conditions such as coagulopathies, diabetes, or peripheral vascular disease may have impaired microcirculation (Papachristos & Giannoudis, 2019). The entire surgical team must pay careful attention to any patient specific conditions that can make them more prone to developing compartment syndrome.
Early diagnosis and treatment of compartment syndrome can prevent irreversible damage to the patient. Preoperative assessment should identify patients at higher risk of compartment syndrome and facilitate planning to mitigate these risk factors. Intraoperative measures include careful patient positioning to avoid prolonged pressure on extremities and limited use of tourniquets (Halvachizdeh et al., 2017). The surgical team should also avoid excessive fluid administration and use careful dissection techniques to minimize tissue trauma. Postoperative monitoring is essential to regularly assess the limb compartments. Some symptoms include severe pain, skin changes, decreased pulses, decreased two-point discrimination, and affected motor function. Measuring intracompartmental pressures of the affected body part can also help diagnose compartment syndrome, and an intracompartmental pressure greater than 30 mmHg will require prompt intervention (Torlincask et al., 2023).
Ultimately, compartment syndrome is a very serious condition that requires high levels of suspicion in patients and procedures with increased risk factors, early detection in the perioperative setting, and rapid treatment. While compartment syndrome is primarily associated with trauma and certain types of injuries, it is important to recognize that it can occur in the surgical environment as well. Ongoing education is essential to ensuring optimal patient safety and health outcomes.
References
Garner MR, Taylor SA, Gausden E, Lyden JP. Compartment syndrome: diagnosis, management, and unique concerns in the twenty-first century. HSS J. 2014;10(2):143-152. doi:10.1007/s11420-014-9386-8
Halvachizadeh S, Jensen KO, Pape HC. Compartment Syndrome Due to Patient Positioning. 2019 Sep 3. In: Mauffrey C, Hak DJ, Martin III MP, editors. Compartment Syndrome: A Guide to Diagnosis and Management [Internet]. Cham (CH): Springer; 2019. Chapter 12. Available from: https://www.ncbi.nlm.nih.gov/books/NBK553906/ doi: 10.1007/978-3-030-22331-1_12
Papachristos IV, Giannoudis PV. Unusual Presentation of Compartment Syndrome. 2019 Sep 3. In: Mauffrey C, Hak DJ, Martin III MP, editors. Compartment Syndrome: A Guide to Diagnosis and Management [Internet]. Cham (CH): Springer; 2019. Chapter 15. Available from: https://www.ncbi.nlm.nih.gov/books/NBK553896/ doi: 10.1007/978-3-030-22331-1_15
Torlincasi AM, Lopez RA, Waseem M. Acute Compartment Syndrome. [Updated 2023 Jan 16]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK448124/